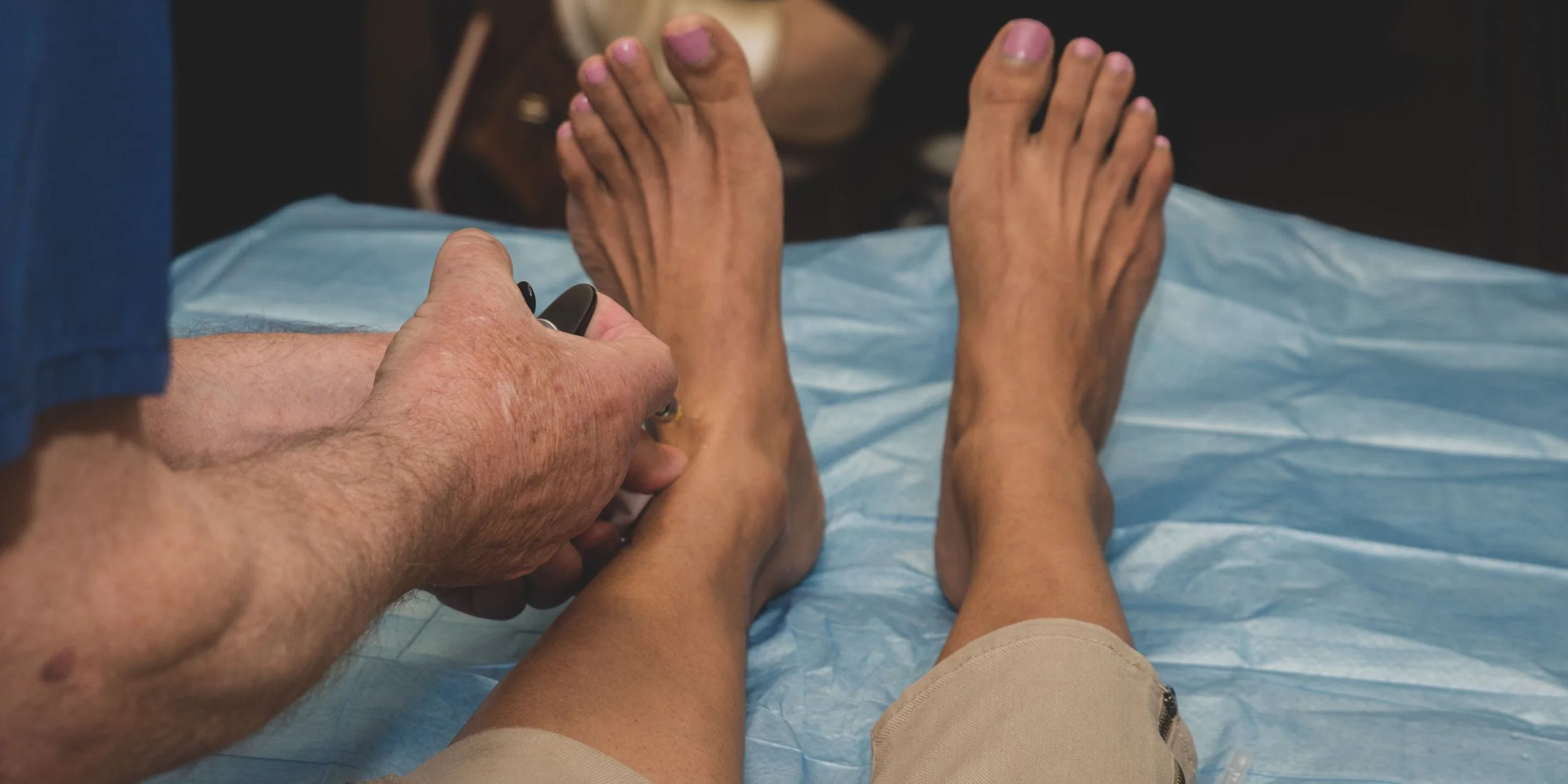
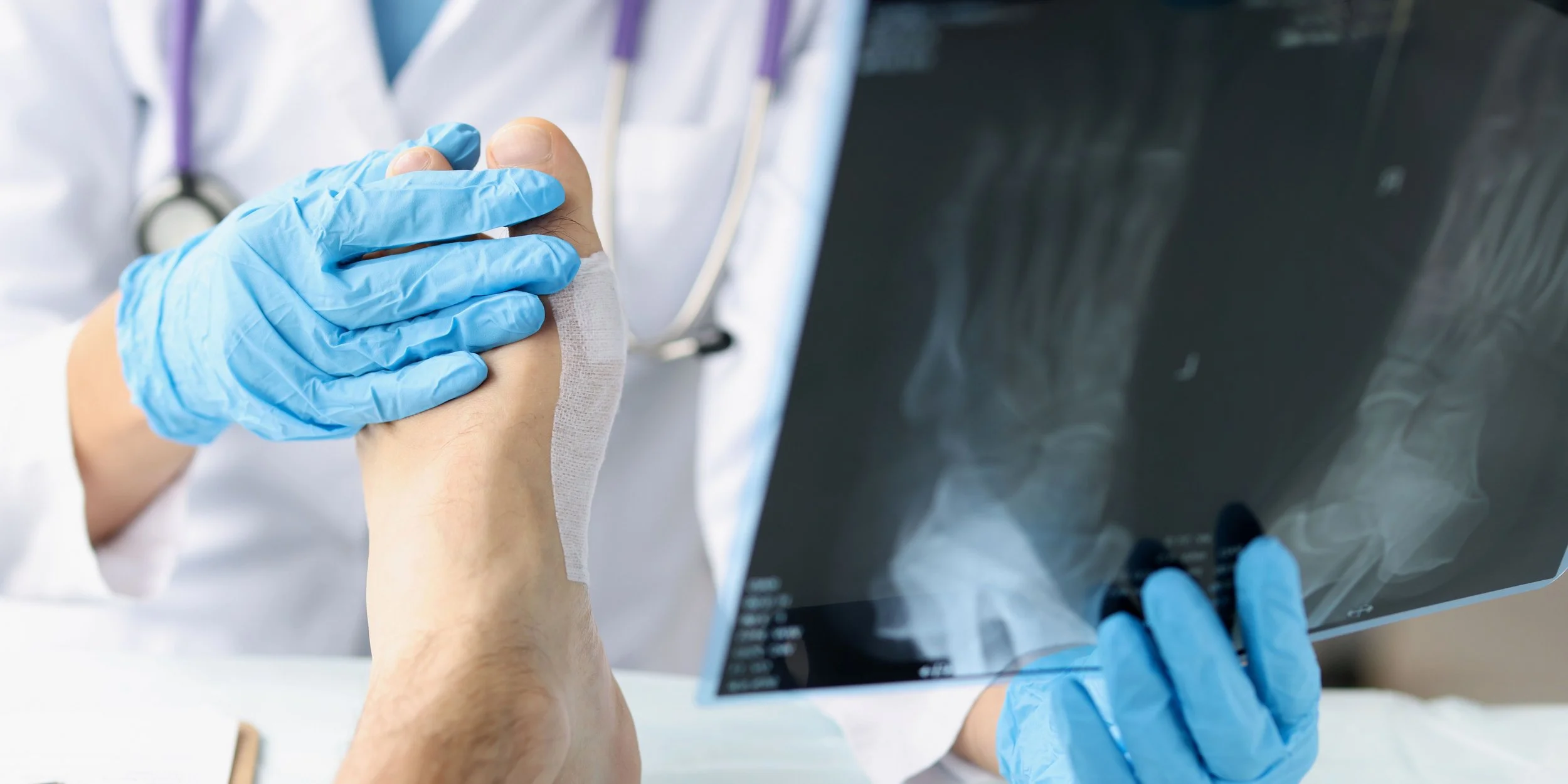
Less Pain, Smaller Incisions, Faster Recovery: The Truth About MIS
You've probably been putting this off.
Maybe your bunion has been bothering you for years. Maybe you’ve tried wider shoes, inserts, toe spacers, orthotics — all the usual things. Maybe surgery came up once during an appointment and you immediately thought, “Nope.”
I get it.
Most people still picture foot surgery as a big incision, weeks off their feet, months in a boot, and a long painful recovery. And for a long time, that was the reality for many procedures.
But minimally invasive foot surgery has changed a lot about that experience.
A lot of my patients are surprised when they realize they’re walking much sooner than expected, and that recovery is often more manageable than what they had built up in their minds. That doesn’t make it “easy,” and it doesn’t make everyone a candidate. But for the right patient, it can change the decision entirely.
Here’s what I want people to understand before waiting another year.
The Problem With “Just Living With It”
Bunions, hammertoes, and bone spurs usually don’t stay the same over time.
A mild bunion can slowly become more severe. Toes become more rigid. Joints become more irritated. A lot of patients also start changing the way they walk without realizing it, which can eventually affect the knees, hips, and lower back too.
People normalize foot pain for years. They stop wearing certain shoes. They avoid long walks. They stand less. They adjust little parts of daily life around their feet until it becomes their normal.
I understand why people wait. Most patients are trying to avoid a recovery they’ve heard horror stories about.
But delaying treatment can sometimes make surgery more complicated later. By the time some patients finally come in, the deformity is more advanced and there are additional problems that developed along the way.
That doesn’t mean everyone needs surgery right away. But it’s important to understand that these conditions are usually progressive, not static.
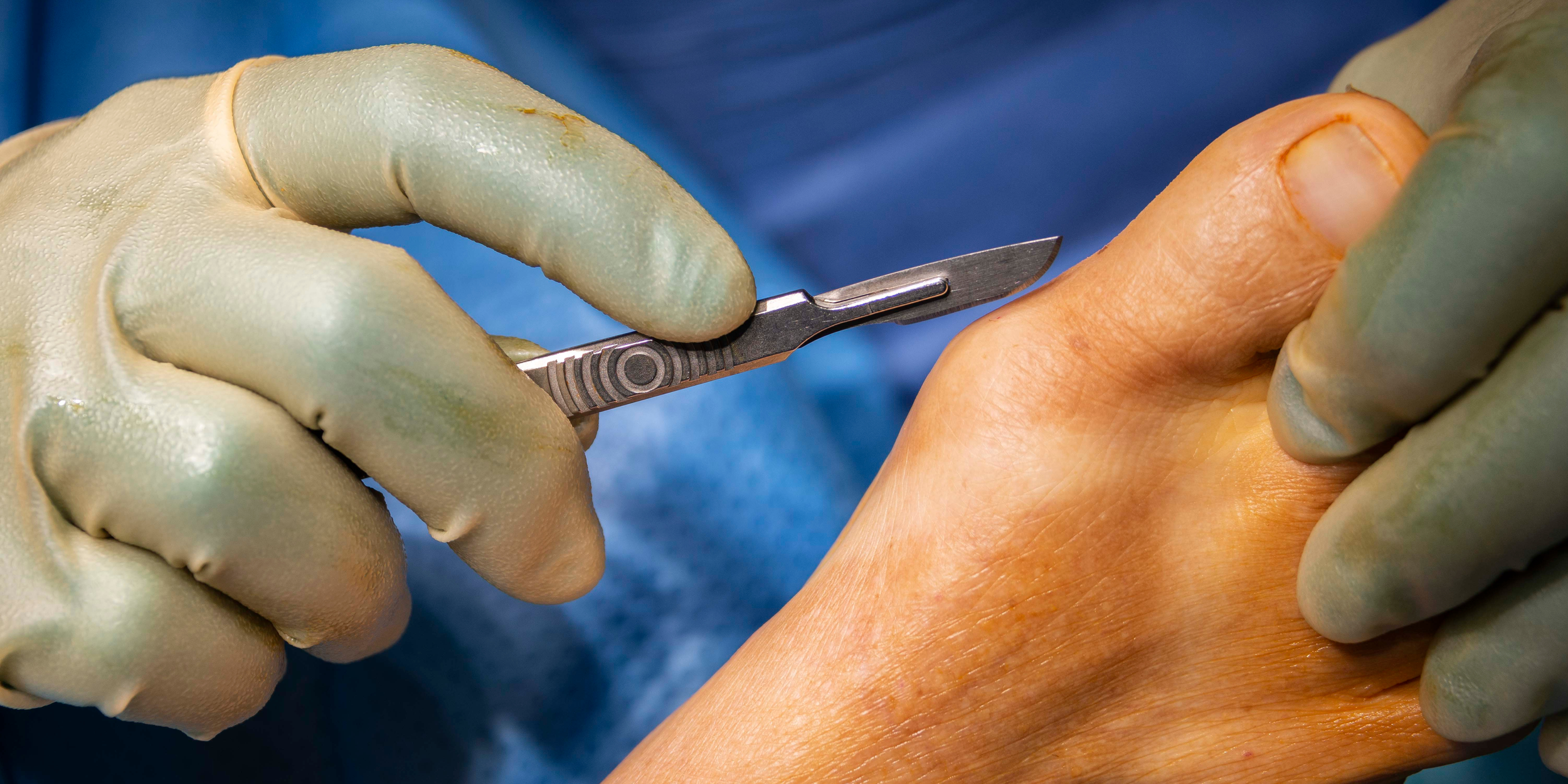
What Minimally Invasive Foot Surgery Actually Is
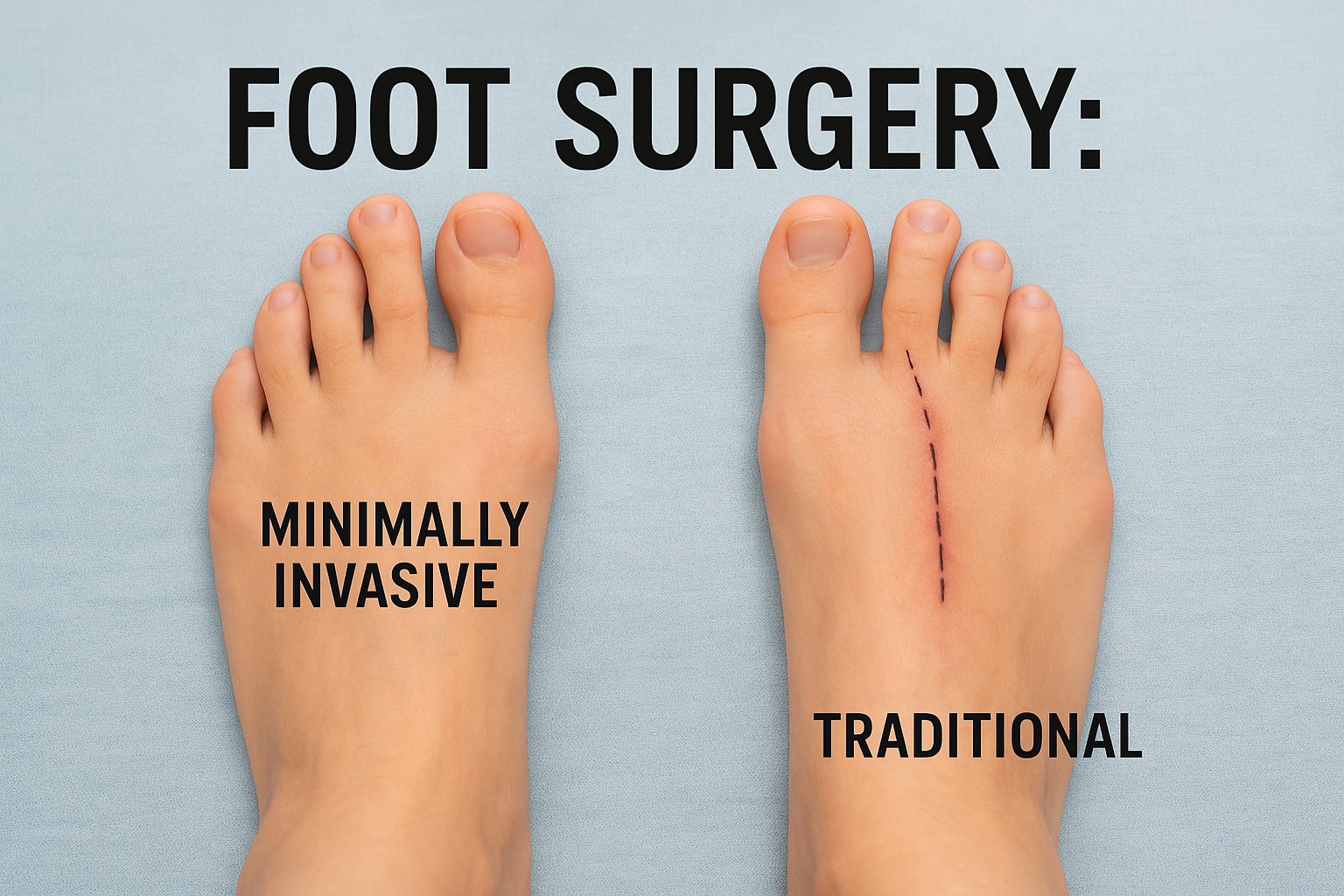
Traditional foot surgery uses a larger incision to directly access the area being corrected. It works well in the right cases, but it does involve more disruption to the surrounding soft tissue. And that disruption is a big part of the swelling and soreness people associate with surgery.
Minimally invasive foot surgery (MIS) is different in how we get to the same problem.
Instead of one larger incision, we use several very small ones — often just a few millimeters. With specialized instruments and imaging, we’re able to correct the deformity while limiting tissue disruption.
The goal is still the same. The bone still gets repositioned. The alignment still gets corrected.
The difference is how we get there.
And in many cases, less disruption means less swelling, less pain, and a smoother recovery.
It’s important to say this clearly: MIS is not a simpler version of surgery. It takes training, experience, and the right patient selection. But when it’s appropriate, outcomes can be excellent.
Conditions MIS Can Treat
Minimally invasive techniques can be used for a wide range of common foot problems.
Bunions (Hallux Valgus)
Bunions are one of the most common conditions treated with minimally invasive surgery. The metatarsal bone is carefully repositioned through small incisions to correct the alignment of the big toe and reduce the prominence of the bunion.
A lot of patients have spent years trying to manage bunions with padding, shoe modifications, or orthotics. Sometimes those things help temporarily, but they don’t actually correct the underlying deformity.
MIS allows us to address the structural problem itself while typically making recovery easier than patients expect.
Hammertoes
Hammertoes happen when one or more smaller toes become bent at the joint over time. This can lead to pain, corns, rubbing in shoes, and difficulty finding comfortable footwear.
Using minimally invasive techniques, we can often rebalance the toe and correct the deformity through very small incisions, with less stiffness and scar tissue afterward compared to traditional open approaches.
Bone Spurs
Bone spurs can develop on the heel, top of the foot, or around joints and create significant irritation with activity or certain shoes.
Minimally invasive surgery can often remove these areas of irritation through small incisions, allowing patients to get back into regular footwear sooner than they expect.
Tailor’s Bunions (Bunionettes)
A tailor’s bunion forms along the outside of the foot near the pinky toe. Just like a traditional bunion, this deformity can become increasingly painful over time, especially in tighter shoes.
MIS techniques can often correct this with the same lower-disruption approach used for standard bunions.
Other Toe and Forefoot Conditions
Minimally invasive techniques may also be appropriate for certain crossover toes, mallet toes, and other forefoot deformities.
The best way to know whether
What Recovery Actually Looks Like
For most patients, this is the question that matters most.
Recovery after traditional open foot surgery can be significant. Depending on the procedure, patients may spend several weeks non-weight-bearing, followed by time in a boot before gradually transitioning back into regular shoes.
With minimally invasive foot surgery, recovery often looks very different.
Many patients are walking in a surgical shoe within days of surgery. Swelling is usually more manageable because there’s less disruption to the surrounding tissue. A lot of patients transition back into wider regular shoes around the six- to eight-week mark, depending on healing and the specific procedure performed.
Low-impact activity often resumes sooner than patients expect, although healing timelines still vary from person to person.
And that part matters.
Even with minimally invasive surgery, bones still need time to heal correctly. The goal is never just a fast recovery. The goal is a stable correction that holds up long term.
But one of the biggest things patients tell me afterward is this:
“If I knew recovery would be like this, I would’ve done it sooner.”
The Pain Difference
One of the biggest fears patients have about foot surgery is pain.
And honestly, most people expect it to be much worse than it actually is.
Smaller incisions generally mean less soft tissue disruption. Less tissue disruption usually means less inflammation, which often translates to less pain during recovery.
That doesn’t mean patients have no discomfort. This is still surgery, and recovery should still be taken seriously. But many minimally invasive surgery patients describe the first week as manageable and much less intense than they anticipated.
And practically speaking, this matters.
Less pain usually means patients are moving around sooner, sleeping better, and needing less help at home during recovery. For patients with jobs, families, or busy schedules, that can make surgery feel much more realistic than they originally thought.
What Open Surgery Still Does Better
Honest medicine means saying this clearly: minimally invasive surgery is not the right option for every patient.
And honestly, if a surgeon tells you otherwise, I’d be cautious.
Some severe deformities — especially cases involving advanced arthritis, major instability, revision surgery, or joint fusion — may still be better treated with open surgery or a combination approach.
Sometimes open surgery truly is the best option for achieving a stable, long-term correction.
That’s why a proper surgical consultation matters. Weight-bearing X-rays, bone quality, joint condition, overall foot structure, and medical history all factor into deciding which approach makes the most sense.
The goal should never be to push one technique over another.
The goal is choosing the right procedure for the right patient.
What minimally invasive surgery has changed is that many patients who used to avoid surgery because of the recovery now have another option worth considering.
Why Patients Wait
There are a lot of reasons patients put this off.
Some people were told years ago that their bunion “wasn’t bad enough yet.” Others had friends or family members who went through difficult recoveries with older surgical techniques. Some patients are just busy taking care of everyone else and keep pushing their own pain down the priority list.
And some genuinely don’t realize how much their feet have started affecting their daily life until we talk through it together.
I hear this all the time:
“I didn’t realize how much I had adjusted around the pain.”
That’s usually the point where patients start seriously considering treatment.
Not because the deformity suddenly got worse overnight, but because they finally realize how much it’s been limiting them.
Take the Next Step
If you’ve been living with bunion pain, hammertoes, or other foot problems and wondering if surgery is something you should actually consider, the next step is simple — get the information first.
We’ll look at your X-rays, talk through what you’re feeling, and go over what treatment would realistically look like for your specific case. Including recovery. Including downtime. Including whether surgery even makes sense for you right now.
No pressure. No assumptions. Just a clear conversation so you can make a decision with real information instead of guessing or waiting in uncertainty.
And if it turns out you’re not ready for surgery, that’s fine too. At least you’ll know where things stand.
The consultation is just a starting point.
Waiting doesn’t make the problem go away — it just makes the decision harder later.